Have you ever wondered how your cardiologist sees inside your heart arteries in such incredible detail? Optical coherence tomography (OCT) is one of the most advanced imaging technologies available in modern cardiology — an "ultra-high definition camera" that uses light to create crystal-clear images of your coronary arteries.
Here's the key insight: OCT provides 10 times more detail than IVUS (intravascular ultrasound), revealing features invisible to any other imaging technique. Research shows OCT-guided procedures reduce stent thrombosis by 51% and cardiovascular death by 44%.
In This Article
What Is Optical Coherence Tomography (OCT)?
Optical coherence tomography uses near-infrared light to create detailed images of the inside of your coronary arteries. If you've heard of IVUS (intravascular ultrasound), OCT takes things to another level — while IVUS uses sound waves like a regular ultrasound, OCT uses infrared light similar to how your smartphone camera captures incredibly detailed photos.
The 4K Ultra-HD Analogy
Think of upgrading from a standard TV to a 4K ultra-HD screen. Regular angiography is like standard definition — you see the basic picture. IVUS is like high definition — much better. OCT is like 4K ultra-HD — suddenly you can see every tiny detail that was completely invisible before.
This gives OCT the ability to see details that are 10 times smaller than what IVUS can detect. The resolution is so fine (10-20 micrometers) that doctors can see individual layers of the artery wall and even microscopic features of plaque.
How Does OCT Work?
OCT works using a principle called "near-infrared light interferometry" — but here's the simple version:
The Fiber-Optic Camera Analogy
Imagine a tiny fiber-optic camera, thinner than a strand of spaghetti, that can travel inside your blood vessels. This camera shines infrared light onto the artery walls and measures how the light bounces back. Different tissues reflect light differently, creating an incredibly detailed picture.
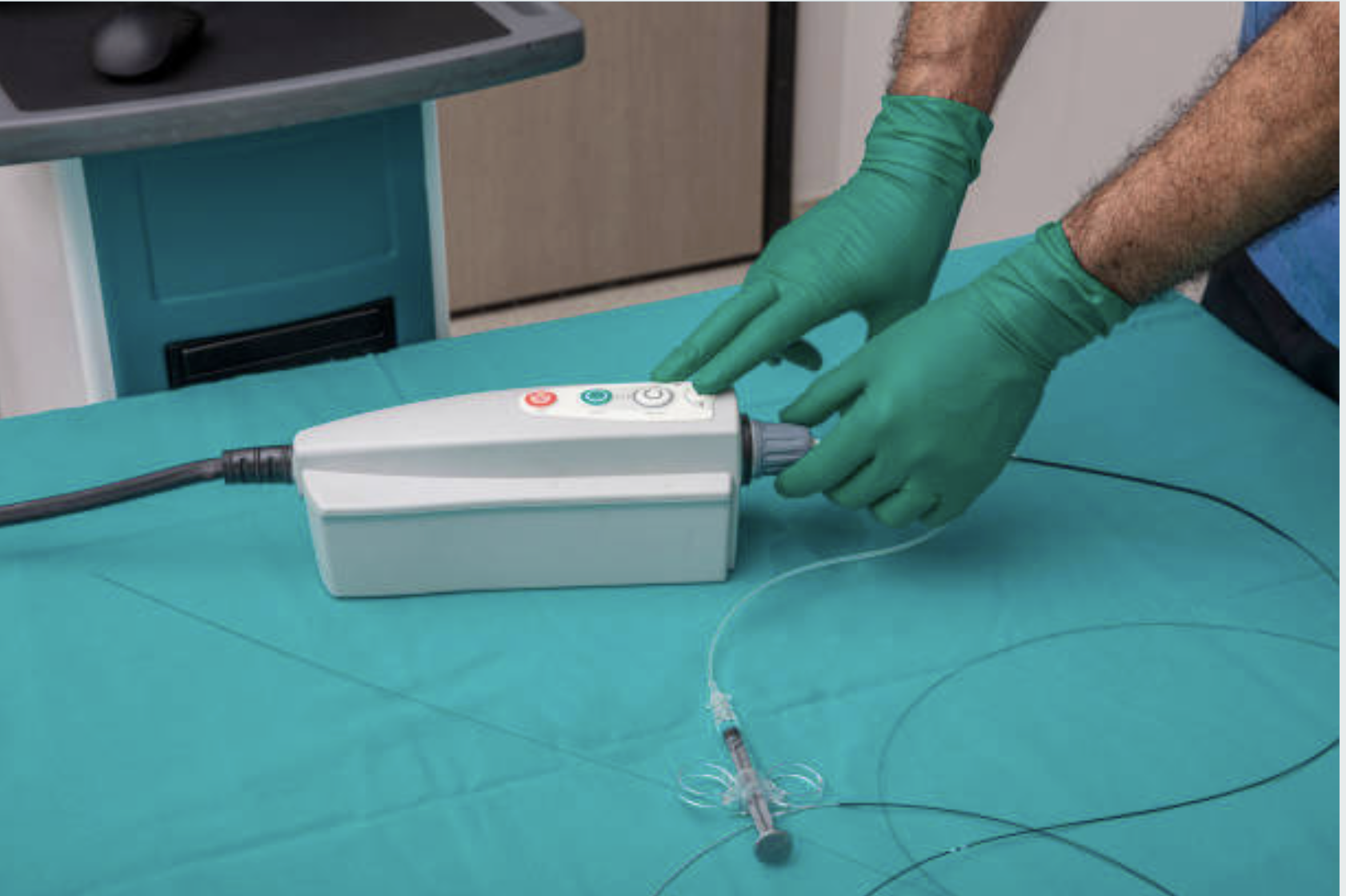
The OCT imaging system: The thin catheter connects to a pullback device that records images as it withdraws through the artery.
The Process Step-by-Step
1. Catheter insertion
A thin catheter (about 2.7mm) is inserted through your wrist or groin — the same entry point used for angioplasty
2. Position the OCT catheter
The OCT catheter travels to the area of concern in your heart arteries
3. Clear the blood
Blood is temporarily cleared by flushing contrast dye (the same dye used in angiography)
4. Light pulses scan
Light pulses scan the artery wall as the catheter pulls back
5. 360-degree image created
A complete cross-sectional image is created in just 2-3 seconds
Incredible Detail
The result? Your cardiologist gets a cross-sectional view of your artery with resolution down to 10-20 micrometers (that's 10-20 millionths of a meter!). For comparison, a human hair is about 70 micrometers wide.
What Can OCT Show That Other Tests Cannot?
OCT's exceptional image quality allows your cardiologist to see things that are invisible on regular angiography or even IVUS:
1. Plaque Composition and Type
Not all blockages are the same. OCT can distinguish between:
Lipid-rich plaques
Soft, fatty deposits that may be vulnerable to rupture
Fibrous plaques
Stable, scar-like tissue
Calcified plaques
Hard, calcium-containing deposits
Thin-cap fibroatheromas
Dangerous plaques with thin covering that could rupture

Real OCT imaging: A cross-sectional view showing the artery lumen (dark center) and wall layers with incredible detail. Different tissue types appear in different shades.
2. Precise Calcium Assessment
If your arteries have calcium buildup, OCT can precisely measure:
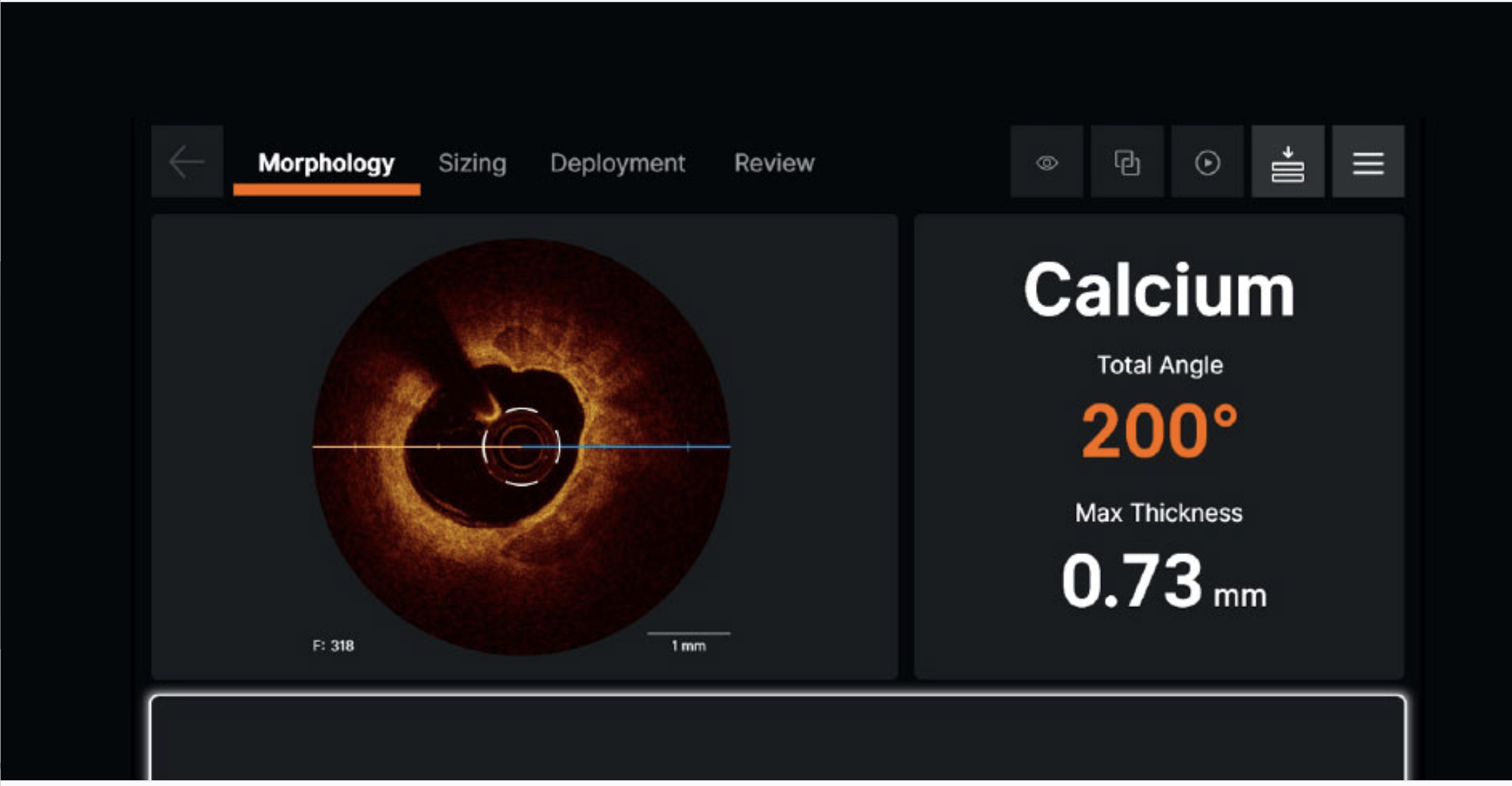
OCT calcium analysis: The console shows calcium arc (200°) and maximum thickness (0.73mm) — precise measurements that guide treatment decisions.
Calcium arc: How much of the artery circumference is covered (measured in degrees, like a slice of pie)
Calcium thickness: How deep the calcium extends into the artery wall
Calcium length: How far the calcium stretches along the artery
This information is crucial for deciding whether you need special tools like rotational atherectomy or intravascular lithotripsy to prepare the artery before stenting.
3. Stent Assessment
After a stent is placed, OCT can show:
- • Stent expansion: Is the stent fully opened?
- • Stent apposition: Is the stent pressing properly against the artery wall?
- • Edge dissections: Are there any tears at the edges of the stent?
- • Tissue coverage: Months later, has healthy tissue grown over the stent?
4. Heart Attack Cause Identification
When someone has a heart attack, OCT can identify the exact cause:
- • Plaque rupture: When a fatty plaque breaks open
- • Plaque erosion: When the surface lining wears away
- • Calcified nodule: When calcium protrudes into the artery
- • Spontaneous dissection: When the artery wall tears
When Do Doctors Use OCT?
Your interventional cardiologist may recommend OCT in several situations:
Before Angioplasty
- • Assessing blockage severity when angiography is unclear
- • Understanding plaque composition to plan the procedure
- • Measuring vessel size for accurate stent selection
- • Evaluating calcium burden to decide on preparation strategy
During Angioplasty
- • Guiding stent placement for optimal positioning
- • Checking for complications like edge dissections
- • Ensuring complete stent expansion
- • Confirming good wall contact (apposition)
For Special Situations
- • Left main artery disease: Where precision is critical
- • Long or complex lesions: Multiple stents needed
- • Stent problems: Re-blockage or suspected stent thrombosis
- • Spontaneous coronary artery dissection (SCAD)
OCT vs IVUS: Which is Better?
Both OCT and IVUS are excellent imaging tools, and often the choice depends on the specific situation. Here's how they compare:
| Feature | OCT | IVUS |
|---|---|---|
| Resolution | 10-20 μm (ultra-high) | 100-150 μm (high) |
| Penetration depth | 1-2 mm | 4-8 mm |
| Blood clearing | Required (contrast flush) | Not required |
| Calcium detection | Excellent detail | Good but less precise |
| Plaque characterization | Superior | Good |
| Stent assessment | Excellent (sees struts) | Excellent |
| Best for | Detail, calcium, stent complications | Large vessels, deeper structures |
What Research Shows
A major 2024 network meta-analysis published in Circulation analyzed 24 clinical trials involving over 15,000 patients:
15,489 patients
Analyzed across 24 randomized trials comparing angiography, IVUS, and OCT guidance.
| Outcome | OCT vs Angiography |
|---|---|
| Stent thrombosis | 51% reduction |
| Cardiovascular death | 44% reduction |
| Major adverse cardiac events | 21% reduction |
The Bottom Line
Both OCT and IVUS are better than angiography alone. They provide similar overall outcomes when compared head-to-head. Your cardiologist will choose based on your specific anatomy and clinical question.
What to Expect During an OCT Procedure

Getting clear answers about your heart health brings relief and confidence.
Before the Procedure
- • Same preparation as for angiography/angioplasty
- • Local anesthesia at the access site (usually wrist)
- • Mild sedation may be given for comfort
During the Imaging
- • You'll feel the catheter moving, but OCT itself is painless
- • A brief warm flush when contrast is injected (lasts 2-3 seconds)
- • The scan takes only seconds per pullback
- • Multiple pullbacks may be done to image different areas
Important Notes
Time: OCT adds approximately 5-10 minutes to the total procedure time
Contrast: Uses additional contrast dye (typically 10-20 mL per pullback)
Visual: Your doctor may share the images with you — they're quite remarkable to see!
No Radiation
OCT uses infrared light (similar to a TV remote), not X-rays. The OCT imaging adds no radiation exposure at all.
Frequently Asked Questions
Is OCT painful? ▼
No, OCT itself is completely painless. You may feel a brief warm sensation during the contrast flush (lasting 2-3 seconds), but the light-based imaging causes no discomfort at all. Most patients don't even notice when the OCT scan is happening.
How long does OCT add to my procedure? ▼
OCT typically adds 5-10 minutes to your angioplasty or stent procedure. The actual imaging takes only seconds, but positioning the catheter and analyzing images adds a little time. This small investment often prevents complications and improves long-term results.
Is OCT safe for patients with kidney problems? ▼
OCT does require contrast dye, but much less than standard angiography — typically 10-20 mL per scan. Your cardiologist will consider your kidney function when planning the procedure. For patients with significant kidney issues, they may limit the number of pullbacks or choose alternative imaging strategies.
Why didn't my doctor use OCT during my procedure? ▼
OCT isn't necessary for every procedure. Your doctor considers several factors: the complexity of your blockage, whether they need more information than angiography provides, and the specific clinical questions. For straightforward cases, experienced cardiologists can achieve excellent results with angiography alone. OCT is most valuable in complex situations where extra detail helps.
How is OCT different from a CT scan of my heart? ▼
CT angiography and intravascular OCT are completely different tests. CT scans your heart from outside your body and shows the overall anatomy. OCT is performed during cardiac catheterization, traveling inside your arteries to provide microscopic detail of the vessel wall. Think of CT as a satellite view of a city, while OCT is like walking through the streets with a magnifying glass.
Can OCT tell if my stent is working properly? ▼
Absolutely — this is one of OCT's greatest strengths. It can show whether your stent has expanded fully, whether it's sitting properly against the artery wall, and whether healing tissue has covered the stent struts. If you're having problems months or years after stenting, OCT can reveal issues like incomplete healing, new tissue growth inside the stent, or new blockages at the stent edges.
Does OCT expose me to radiation? ▼
No, OCT uses infrared light (similar to the light in a TV remote), not X-rays or radiation. The regular angiography portion of your procedure does use X-rays, but the OCT imaging adds no radiation exposure at all.
Is OCT available in India? ▼
Yes, OCT is available at most major cardiac centers and hospitals with interventional cardiology programs. In India, most large hospitals in metropolitan areas offer OCT imaging. Both our Fortis locations in Delhi — Shalimar Bagh and Vasant Kunj — have OCT capability.
Life After Your Procedure

Understanding your heart care empowers you to live life confidently.
When you're facing a heart procedure, it's natural to want the best possible care. OCT represents one way that modern cardiology has moved beyond simple X-ray guidance to sophisticated imaging that improves outcomes.
If you have questions about whether OCT might be used in your procedure, ask your cardiologist. They can explain their approach and why certain imaging techniques are recommended for your specific situation.
References
- Giacoppo D, et al. Coronary Angiography, Intravascular Ultrasound, and Optical Coherence Tomography for Guiding of Percutaneous Coronary Intervention: A Systematic Review and Network Meta-Analysis. Circulation. 2024;149(14):1065-1086. PMID: 38344859
- Wang Y, et al. Optical coherence tomography (OCT)- versus angiography-guided strategy for percutaneous coronary intervention: a meta-analysis of randomized trials. BMC Cardiovasc Disord. 2024;24(1):262. PMID: 38769510
- Truesdell AG, et al. Intravascular Imaging During Percutaneous Coronary Intervention: JACC State-of-the-Art Review. J Am Coll Cardiol. 2023;81(6):590-605. PMID: 36754518
- Karimi Galougahi K, et al. Utility of optical coherence tomography in acute coronary syndromes. Catheter Cardiovasc Interv. 2023;102(1):46-55. PMID: 37245076
- Volleberg R, et al. Optical coherence tomography and coronary revascularization: from indication to procedural optimization. Trends Cardiovasc Med. 2023;33(2):92-106. PMID: 34728349
- Vats V, et al. Optical coherence tomography-guided vs. intravascular ultrasound-guided percutaneous coronary intervention: a systematic review and meta-analysis. Front Cardiovasc Med. 2024;11:1395606. PMID: 38883988

About the Author
Dr. Shailesh Singh is a Senior Consultant Interventional Cardiologist with over 12 years of experience in complex coronary interventions. He practices at Fortis Hospital Shalimar Bagh and Fortis Hospital Vasant Kunj in Delhi, where he uses advanced imaging techniques including OCT to optimize patient outcomes.
Learn more about Dr. Singh →Questions About Your Heart Procedure?
Dr. Shailesh Singh uses advanced imaging techniques including OCT to ensure the best possible outcomes for his patients. Book a consultation to discuss your cardiac care.
Locations: Fortis Shalimar Bagh | Fortis Vasant Kunj
Medical Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Please consult with your cardiologist about your specific condition and treatment options.